The purpose of this letter is to explain what is involved when a fusion is performed on your lower back. We have found that the more knowledgeable the patient, the more successful the outcome. This letter is intended to answer some of the most commonly asked questions. Please feel free to raise any other questions with your doctor.
- What is the basic structure of the spine?
The spine is composed of vertebrae, disks, spinal cord and nerves. Typically, the vertebrae are referred to as the “spine”. These vertebrae are bones that support the trunk and protect the spinal cord and nerves. The disk is the soft structure located between the vertebrae. The disks act as cushions, which enable the vertebrae to move.
- What is a lumbar fusion?
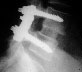 A lumbar fusion is when two or more vertebrae in the low back are “welded” together to create a solid bridge of bone between the vertebrae and across the disc space. A fusion is usually performed to eliminate movement between vertebrae and stabilize a painful or unstable segment of the spine. Once a segment of the spine is stabilized, the patient usually experiences some relief of pain. Surgery is not usually recommended unless there is a more than 70% chance of improving the level of pain. This approximately 70% chance of improvement does not necessarily mean you will be completely pain free but rather that your level of pain should be significantly improved. It means that there may be a significant chance your pain will not improve. However, each situation is unique. There is also a small chance that you may become significantly worse.
A lumbar fusion is when two or more vertebrae in the low back are “welded” together to create a solid bridge of bone between the vertebrae and across the disc space. A fusion is usually performed to eliminate movement between vertebrae and stabilize a painful or unstable segment of the spine. Once a segment of the spine is stabilized, the patient usually experiences some relief of pain. Surgery is not usually recommended unless there is a more than 70% chance of improving the level of pain. This approximately 70% chance of improvement does not necessarily mean you will be completely pain free but rather that your level of pain should be significantly improved. It means that there may be a significant chance your pain will not improve. However, each situation is unique. There is also a small chance that you may become significantly worse.
- Will I lose mobility once a portion of spine becomes solid bone?
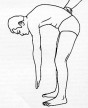 It depends in part on how much of the spine is fused. The spine will not move as much but you may not notice it because it is a small percent of your spine. Most believe that the spine enables you to bend over at the waist. This motion actually occurs mostly at the hips. There are patients who have their entire spines fused yet are still able to touch their fingertips to the floor.
It depends in part on how much of the spine is fused. The spine will not move as much but you may not notice it because it is a small percent of your spine. Most believe that the spine enables you to bend over at the waist. This motion actually occurs mostly at the hips. There are patients who have their entire spines fused yet are still able to touch their fingertips to the floor.
- What happens during an anterior lumber fusion?
 At the hospital you are taken to the Transfer Area, where an anesthesiologist explains the anesthesia process. You are than taken to the Operating Room and given a general anesthetic to put you to sleep. After you are asleep you are carefully positioned on the table. You may be positioned on your side or on your back, depending on the needs of your particular case. An incision is made through the abdominal muscles. This incision may be directly in front of your abdomen and may be straight, horizontal, or vertical; sometimes it is more towards your flank and somewhat diagonal in direction; depending on which level of your spine needs to be fused and the number of levels involved. The surgery is then done by moving the abdominal contents over and then identifying the great vessels called the aorta and the inferior vena cave.
At the hospital you are taken to the Transfer Area, where an anesthesiologist explains the anesthesia process. You are than taken to the Operating Room and given a general anesthetic to put you to sleep. After you are asleep you are carefully positioned on the table. You may be positioned on your side or on your back, depending on the needs of your particular case. An incision is made through the abdominal muscles. This incision may be directly in front of your abdomen and may be straight, horizontal, or vertical; sometimes it is more towards your flank and somewhat diagonal in direction; depending on which level of your spine needs to be fused and the number of levels involved. The surgery is then done by moving the abdominal contents over and then identifying the great vessels called the aorta and the inferior vena cave.
![]() These are carefully retracted over the spine. At this point, we are able to look directly at the front part of the spine and have an excellent look at the disc spaces. The size of the graft or interbody device is carefully matched to fit into the spaces between your vertebrae. This is then impacted into place, to try to give it as firm a fit as possible.
These are carefully retracted over the spine. At this point, we are able to look directly at the front part of the spine and have an excellent look at the disc spaces. The size of the graft or interbody device is carefully matched to fit into the spaces between your vertebrae. This is then impacted into place, to try to give it as firm a fit as possible.
There is now new technology for spinal fusion using interbody device technology.
When the interbody devices are used, the bone graft or bone graft substitute is put inside a hollow space within the device. Whether or not an interbody device is used to support bone grafting, the principles are the same. Over time the body will turn the bone graft or substitute into a solid piece of bone and eliminate the movement between the vertebrae.
- How is an anterior lumber fusion different from a posterior lumbar fusion?
 In a posterior lumbar fusion, the fusion is done through the back part of the spine. The muscles are dissected from the spine. The bony surfaces of the spine are exposed and small pieces of bone are laid across the back part of the spine. In an anterior fusion, surgery is done through the front part of the spine, which makes it necessary for us to go through your abdomen. Instead of using chips of bone graft to span the space, a solid piece of bone or interbody device is generally used. In the anterior fusion, the bone graft or substitute is packed directly between the vertebral bodies, whereas in the posterior fusion the bone is laid across the back part of the spine. It is generally felt that if one can obtain a solid anterior fusion there is a mechanical advantage, in that most of the forces on the spine are transmitted through the front part of the spine.
In a posterior lumbar fusion, the fusion is done through the back part of the spine. The muscles are dissected from the spine. The bony surfaces of the spine are exposed and small pieces of bone are laid across the back part of the spine. In an anterior fusion, surgery is done through the front part of the spine, which makes it necessary for us to go through your abdomen. Instead of using chips of bone graft to span the space, a solid piece of bone or interbody device is generally used. In the anterior fusion, the bone graft or substitute is packed directly between the vertebral bodies, whereas in the posterior fusion the bone is laid across the back part of the spine. It is generally felt that if one can obtain a solid anterior fusion there is a mechanical advantage, in that most of the forces on the spine are transmitted through the front part of the spine.
- When is an anterior fusion chosen instead of a posterior fusion?
An anterior fusion is chosen for several reasons. Your surgeon may feel that with the new device technology and your particular situation that an anterior fusion is a better way to obtain a fusion. However, anterior fusion is also used in addition to a posterior fusion to improve the fusion rate. In certain spinal deformity situations, multiple discs are removed from the front of the spine to “loosen up” the spine and improve the correction of deformity.
- What are interbody devices or Cages?
A cage is a synthetic device of various shapes with or without threads that is placed within the disc space. There are special tools to create the appropriate holes in the front part of the spine and then the threaded cylinders are screwed into the spine. The vertebrae are being held apart by a hollow device (the cage) that has holes on the outside. The bone graft is then packed into the middle part of this device and there is direct contact between the rough bony surfaces of the vertebrae and the bone graft through the holes that are on the outside of the device. This contact allows the fusion to occur. There are several brands of cages, but they all use the same principles. They may be made of different types of materials, such as carbon or titanium.
- Why are cages used?
Once the interbody devices are inserted, they provide increased stability to the spine. This seems to improve the back pain quite quickly, as there is very little motion between the vertebrae after the device is in place. It has also been documented that the fusion rate seems to be quite high. Without the devices, historically the fusion rate has been around 60-70%. It is felt that the fusion rate with the devices is over 90%. Another important reason to use the devices is that the bone graft comes in smaller pieces and can be placed inside the device. There seems to be less pain at the bone graft donor site long-term if small pieces of bone are taken from the pelvis, rather than a large block of bone.
- Are there specific risks in using the devices?
There are several risks of anterior lumbar fusions that we will discuss below. The only additional risk of using the device in anterior lumbar fusion is that if the device is placed too far backwards or too far to the side it can damage a nerve root. This is a rare complication and can be solved if the device is removed. If the fusion does not take and the device must be removed, then this can be a challenging procedure. Often, however, the nonunion can be solved by doing a procedure from the back and leaving the device in place.
- Can the device procedure be done through a laparoscope or other minimally invasive techniques?
Technology does exist whereby these devices can be inserted through multiple small incisions or tube retractors, in the abdomen, as opposed to one large incision. The results look promising and the surgery seems to be a little less painful, but it takes longer to perform as it is not quite as easy to expose the spine through theses techniques. We feel that the main advantage of these techniques is less postoperative pain. We do not feel that they add to the fusion rate. The pros and cons of open versus minimally invasive surgery should be discussed with your physician because there are pros and cons to the use of theses techniques depending on which level of your spine is being fused.
- Does smoking have an effect on my fusion?
Research shows that the healing rate is greater than 90% in non smokers and less than 50%in smokers. It appears what with the device technology the difference is not quite as great but there is still certainly a lower fusion rate in patients who smoke. In addition, there is a higher medical complication rate in patients who smoke. Many surgeons will not perform a fusion in patients who smoke because of the higher rate of nonunion and infection. Physicians have also found that it is sometimes necessary to go through both the front and the back of the spine to obtain a successful fusion in smokers. If you smoke, be prepared to discuss the situation in detail with your physician.
- What will my hospital stay be like?
You will check into the hospital approximately two hours before surgery. Several nurses and doctors will ask you questions regarding your medical history. It would be helpful to bring a list of medications with exact dosages that you are currently using. You will wait in the holding area of the operating room for about 30 minutes before surgery. This is where you will meet your anesthesiologist and have your IV’s initiated.
After surgery you will wake up in the recovery area where you will remain for about two hours. There will be catheter in your bladder. The catheter is usually removed on the 2nd or 3rd postoperative day. However, if you are unable to urinate you may need to be recatheterized. Due to the anesthesia and medications, many patients have a poor recollection of this period.
The first 2 days will be difficult. The most painful part of recovery is usually the abdominal incision and if used, the site of the bone graft harvest. In order to obtain an adequate amount of graft, the muscles inserting into your iliac crest had to be dissected. As you walk these muscles will pull on the graft site. This area will be painful until the scar matures, which may take anywhere from 4 to 6 weeks.
We will try very hard to keep you as comfortable as possible with IV narcotics. You will be able to control the amount of pain medication you receive by using a small push button. You can push the button as often as you need; the machine will control the dose. We have been happy with the amount of pain control we can obtain with this machine.
The combination of narcotics, anesthesia, and the spine surgery may cause you to experience some nausea. We allow only ice chips or small amounts of liquids until you are passing gas. If fed too soon, you may become distended and even more nauseated. About 20% of our patients are fairly nauseated within the first 24 hours. This problem is usually resolved by the second or third day.
We encourage you to get out of bed on the first or second day. By the third day we insist that you are ambulating. We have found that there is a lower incidence of lung, bladder, and vascular complications the earlier you are mobilized.
- When can I go home and what will I be able to do?
You may go home once your pain can be controlled with pills, your incision is not draining, and your bowel and bladder are functioning normally. Most patients are ready to go home by the third or fourth day after surgery.
Within the first few weeks following discharge we encourage you to begin walking for one half hour to two hours each day. If you were given a brace, you must wear it during the day although you can remove it to sleep or shower. You should be able to go up and down stairs, drive, and perform basic daily activities without too much difficulty, within a few weeks of surgery. Driving is not recommended as long as you require frequent narcotic medications for pain control. You should avoid bending or twisting at the waist as that increases the stress across the fusion site. It usually takes a minimum of three to four months for the fusion to heal; most patients are in their braces (if prescribed) for this entire time period. The time frame in which you can return to work depends on your recovery. Each patient has a unique set of work related issues, which will need to be discussed with the doctor.
The first office visit should be scheduled two to four weeks after you are discharged. The purpose of this visit is to check your incision and make sure you are progressing as planned. The second office visit is typically scheduled two to four months after surgery. During this visit the status of your fusion is assessed. Each physician has his own approach to rehabilitation. Your physician will prescribe a rehabilitation program based on your specific needs.
- Will I need a blood transfusion?
A spinal fusion is a major surgery, which may require a blood transfusion. If you are having a one or two level anterior fusion, the blood loss has been shown to be quite minimal. However, if the anterior fusion is being done in conjunction with a posterior fusion, then a blood transfusion may be required. If you require blood, you can donate it yourself or use the hospital blood bank. The blood bank is very safe; the risk of contracting AIDS is less than one in 30,000, and the risk of contracting Hepatitis is one in 10,000. Prior to surgery, our office may arrange pre-donations through the blood bank for those patients who elect to use their own blood.
- What are the specific risks of this operation?
Every surgical procedure carries significant risks. These include major risks, which may have long-term negative side effects and minor risks which do not have long-term effects.
- Major Risks
- Deep Infection 1-2%
These include infections, which may show up several months after surgery and require multiple surgeries and prolonged use of antibiotic. An infection with an anterior fusion is especially difficult to deal with as it is deep in your pelvis and next to major blood vessels.
- Pseudarthrosis 15-40%
A pseudarthrosis or non-union is a term used to describe a fusion that has not healed. This means that a solid bridge of bone has not formed between the vertebrae. A non-union does not necessarily mean that the surgery must be redone; many patients with a non-union are quite happy with their pain relief. However, in cases where the pain persists, the fusion may have to be redone. We have found that smokers, have a higher incidence of pseudarthrosis (>50%) than non-smokers. Therefore, you should be aware that smoking may significantly affect the outcome of your surgery.
- Pulmonary Embolism <5%
Occasionally a blood clot can form in your legs, break off, and travel to your lungs. Once the clot reached the lungs it is referred to as pulmonary embolism, which can be fatal. A pulmonary embolism is rarely found in spine surgery patients. If the clot is detected early it can be treated with blood thinners. The risks are much higher if you have a history of blood clots. Make sure that you inform your doctor of such a history.
- Dural Tear <1%
Generally a dural tear can occur in conjunction with a posterior procedure. It would be unusual to encounter this complication from the front or anterior approach. To heal properly you must remain flat on your back for 24 to 72 hours, so that the leak will seal. If the leak persists, you may require further surgery or special drains.
- Nerve Damage 1-2%
Nerve damage can occur in the front part of the spine if the interbody device is placed too far lateral within the vertebrae. This would put the device within the neural foramin and close to the nerve. This generally causes pain but occasionally causes numbness or weakness in the legs or feel, as well as pain. It would be rare to have a catastrophic complication of lost bowel or bladder function, but it is possible if disc material is pushed straight back into the spinal canal.
- Re-operation 10-20%
Further surgeries may be necessary if the spinal implants break or loosen. Other reasons include nerve impingement from a screw, pseudarthrosis (non-healing of the fusion), infection, or persistent pain.
- Major organ or vessel damage:
With the anterior procedure there is the small additional risk of perforation of the aorta, inferior vena cava, common iliac or other major blood vessel. These are major vessels and injury to them could cause major blood loss. Generally are quickly recognized, stopped in surgery and repaired. In very rare instances, this major bleeding could lead to death. It is also possible to damage the tubes coming from your kidney to your bladder, which would require additional surgery to repair.
- Vascular injury to your legs
As the blood vessels to your legs have to be retracted calcium deposits in your arteries may be dislodged. These deposits can travel to your legs and may occlude the blood supply to your leg or legs. Emergency surgery has to be performed to correct this situation. It may result in partial or complete amputation of your leg.
- Sexual Dysfunction (Males) 2-3%
In males, sterility can occur. This arises from retrograde ejaculation. The male is able to have normal sexual function except that the ejaculate goes backwards into the bladder instead of forwards and out of the penis. There is still full sensation but sterility can occur. Most instances of retrograde ejaculation are temporary, resolve in 6 to 12 months. Occasionally it can be a permanent situation. Impotence (lack of erectile function) is a rare complication of this surgery.
- Persistent pain at the bone graft site 4-5%
Generally the bone graft site seems to have the most pain after surgery. This is because of injury to muscles attached to the pelvis. When you walk this pulls on the area that is sore and irritated. This usually resolves within three to four weeks. Occasionally however, this is a very persistent, long-term problem. We also try to harvest the graft from between the layers of the pelvis to decrease the pain. We also use a synthetic protein which is effective in obtaining a fusion. It is called bone morphogenic protein (BMP) and no bone graft is required.
- Minor Risks
Complications which, are less serious, include bladder infection, superficial wound drainage, inability to urinate for a few days, nausea, headache, constipation, abdominal bloating, sore throat, pneumonia, and reactions to medications. If your body is unable to replenish its blood supply or if too much blood is lost during surgery, a blood transfusion may be necessary. As with any surgery, there are also unanticipated major and minor risks. The lower extremity on the side of the incision may feel warm for varying periods of time due to the “sympathectomy effect”. This symptom usually subsides in a few weeks.
- What is your overall philosophy regarding spinal fusion?
Lumbar fusion is generally an elective surgery. Therefore it is your choice to proceed based on your current level of discomfort and disability. We recommend that you do not have surgery if you can live with your current level of pain or can make changes in your lifestyle to decrease the pain. If you have made a valiant effort and the pain still persists, surgery should be considered.
The rate of surgical success varies greatly depending on your exact problem, overall health, and the magnitude of surgery necessary. We hope that by providing you with as much information as possible about the surgery, you can determine if the pain you are experiencing is worth the risk of surgery.
Theme sponsored by: Adderall website where you can buy Adderall online buyadderall.com and learn about how Adderall and how phentermine works. You can learn about how to buy phentermine online from USA and how phentermine works. Also find out how Modafinil works when you are planning on buying Modafinil online
